Rheumatoid arthritis is a form of arthritis that is a painful degenerative disease that can reduce quality of life. Normally, your immune system protects the body from infections and diseases. However, with an autoimmune disease like rheumatoid arthritis (RA), your immune system is overzealous and mistakenly attacks healthy cells and tissues. Consequently, rheumatoid arthritis has many physical impacts and social consequences.
Apart from severe joint pain and mobility issues, patients with rheumatoid arthritis are also at higher risk of developing other diseases like diabetes and heart disease. In general terms, arthritis means swelling of one or more joints. But the severity of joint stiffness, pain, and complications will vary based on the type of arthritis.
For example, gouty arthritis (which targets a specific joint due to high uric acid food intake) or osteoarthritis (usually the knees due to wear and tear in old age) are less severe forms of arthritis. In contrast, rheumatoid arthritis could start in childhood and result in inflammation not just in the joint linings. Instead, swelling could be present in the whole body and could damage organ tissues like the heart, eyes, or lungs.
Some cases of rheumatoid arthritis will be more severe than others. Both younger and older people can get it. Learn more about this debilitating condition below.
What is Rheumatoid Arthritis?
Rheumatoid arthritis (RA) is an autoimmune inflammatory disease where the immune system mistakenly attacks healthy cells and tissues. As a result, there’s inflammation in the affected body parts resulting in swelling and pain. RA typically attacks multiple joints at the same time, particularly the knees, hands, and wrists.
When the joint lining becomes inflamed due to rheumatoid arthritis, the joint tissue suffers from damage. Halyna Kuzyshyn, board-certified rheumatology and internal medicine doctor, explained that if the tissue remains chronically inflamed, it can lead to the loosening of tendons and ligaments. In turn, this could result in cartilage damage, bone erosion, and loss of function.
When all of these occur, patients can suffer chronic or long-lasting pain, loss of balance, joint deformities, and physical disabilities. For example, patients with severe rheumatoid arthritis have issues with their hands like deformity of thumb, ulnar deviation of finger joints, and swan-like distortion of fingers. In the worst cases, rheumatoid arthritis can affect other tissues, resulting in organ complications, skin issues, nerve problems, and faulty blood vessels.
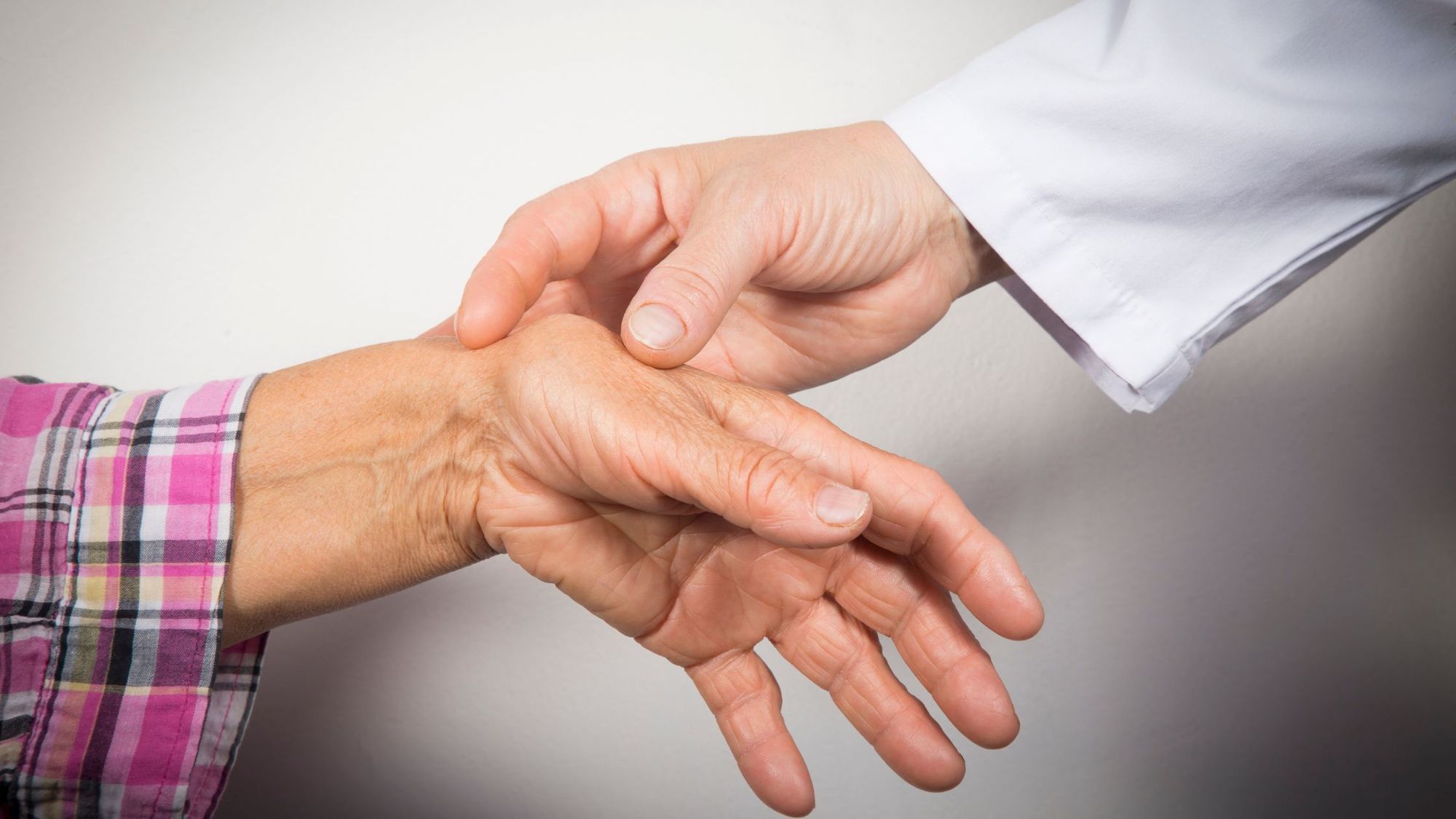
Signs and Symptoms of Rheumatoid Arthritis
Early rheumatoid arthritis begins in smaller joints. Symptoms like warm, tender, and swollen joints start in the joints that attach fingers to the hands and toes to the feet. As the disease progresses, symptoms spread to knees, wrists, ankles, elbows, shoulders, and hips.
For other types of arthritis, symptoms can manifest in one area such as the left knee. But for rheumatoid arthritis, symptoms commonly occur on the same joints on both sides of the body. Common RA symptoms are the following:
- Pain in more than one joint on both sides
- Stiffness in more than one joint, usually worse in the mornings or after inactivity
- Tenderness and swelling in more than one joint
- Loss of appetite
- Weight loss
- Fever
- Fatigue or tiredness
- Problems with mobility (such as being unable to do a long hike)
- Weakness
40% of people who suffer from RA experience symptoms in other areas of the body. Apart from the joints, there could be issues manifesting such as excessively dry skin, faulty heart valves, dryness of the eyes, loss of moisture in the vaginal area, scarring within the lungs, the onset of kidney disease, etc.
Symptoms of rheumatoid arthritis could also vary in severity and may come and go. Periods of painful symptoms are called flare-ups while alternate periods where swelling and pain abate are called remission.
What is the Treatment for this Disease?
Just like most autoimmune diseases such as asthma or psoriasis, there is no cure for rheumatoid arthritis. However, various treatments can slow down the condition. Treatment will involve care from your general practitioner and a rheumatologist, a specialty doctor dealing with immune system-related conditions. They will review symptoms, conduct physical exams, and have x-rays and lab tests done to confirm the disease.
Medication and other supportive treatments are prescribed to reduce inflammation, mitigate the risk of joint damage, and prevent worsening. Usually, DMARDs or disease-modifying antirheumatic drugs and biologicals are given to slow disease progression and limit the impact of RA.
Moreover, self-management with lifestyle changes is also suggested to help mitigate pain and exacerbation. The following strategies could help people with RA pursue activities that matter to them by helping reduce pain:
- Get physically active with joint-friendly exercises like swimming and biking for 150 minutes per week.
- Stop smoking because this makes the disease worse and results in more medical problems.
- Maintain a healthy weight to prevent more undue pressure on the joints.
- Join support groups and self-management education classes to learn how to control symptoms and reduce arthritis flares.
- Watch out for dietary triggers which may result in inflammation such as high fat dairy, refined carbs, gluten, preservatives, and alcohol.
- Eat a complementary diet that supports medications, preferably whole grains, veggies, and fruits.
Risk Factors for Rheumatoid Arthritis
The specific causes of RA are linked to genetic and environmental factors. Characteristics that increase the onset of the disease are the following:
- Genes: RA is heritable and tends to cluster in families. People can be born with specific genes that are likely to result in RA, and they could pass this gene to their children via genetic inheritance. Genes like HLA (human leukocyte antigen) class II genotypes could also make arthritis worse.
- Age: This disease can begin at any age, but the likelihood of onset increases for older people.
- Gender: Unfortunately, rheumatoid arthritis is more prevalent in women at a two to three times higher rate than in men. Women who have also not given birth have a greater risk.
- Smoking: Studies show that smoking increases the risk of RA onset and could make symptoms worse.
- Obesity: Being overweight increases the risk of RA. The higher the weight, the higher the likelihood of onset.
- Early Exposure: Children with early environmental exposure to second-hand smoke have a double risk of developing RA as adults.
Life Complications of Dealing With RA
Rheumatoid arthritis results in drastic changes in everyday life. If you cannot move your joints in their full range of motion because they’re inflamed, this could cause imbalance and poor mobility. The simple things that normal people take for granted like walking, driving, cooking, bending to do laundry, and recreational activities like sports, etc. become challenging with painful, swollen joints. Unfortunately, when you cannot do things that you love and enjoy, this could lead to depression and anxiety.
A study called Everyday Life with Rheumatoid Arthritis points out that joint pain and swelling could result in physical weakness, trouble sleeping, tiredness, reduced mobility, poor self-image, and issues with sexuality (especially for women who have vaginal dryness due to RA). Moreover, those with RA often worry about job security, especially if they have physically demanding jobs because rheumatoid arthritis tends to result in physical limitations. Hence, some patients have had to give up their work or take on a different role due to the pain and loss of strength that accompanies the disease.
Furthermore, someone who is immunocompromised or with a weakened immune system due to rheumatoid arthritis is more prone to illnesses. RA patients have a higher risk of developing other chronic issues like hypertension, diabetes, and heart disease. They are also more prone to communicable diseases. For example, someone with RA may suffer more severe COVID symptoms and be sick for a longer period than a normal person.
Living with rheumatoid arthritis is not easy because it’s difficult to predict when the flares will occur. Symptoms may get better or worse the next day, and there’s no way of knowing ahead. This makes it harder to plan activities because a “bad” day with full-blown pain can incapacitate a person. To make things worse, patients tend to worry and feel anxious about the future, even with medication and support from a rheumatologist, because the disease is unpredictable.
Are You Suffering From Rheumatoid Arthritis or Have the Carrier Gene?
If you have been diagnosed with rheumatoid arthritis, it’s normal to feel worried and concerned because of its potential impact on your life. An early diagnosis and treatment with medication could help reduce your pain and inflammation. It will also improve your physical functioning and could potentially prevent further damage to the joints.
Although rheumatoid arthritis affects many aspects of life including work, social, and leisure activities, you can take comfort in knowing that many RA patients are able to successfully manage symptoms and improve their quality of life. For instance, many follow a clean diet complementary to medication to help control inflammation. Support from family and friends also makes a big difference.
By taking the correct medications and following lifestyle strategies suggested by rheumatologists, many people who have rheumatoid arthritis are able to enjoy days of remission and avoid flares. And if you have a family history of the disease, it’s important to take extra care of your joints by maintaining a healthy weight, eating nutritious meals, and staying active. Avoid alcohol and smoking to promote optimal health.
If you want to stay on top of your health and wellness, consider taking a CircleDNA at-home DNA test. These insightful test results reveal your potential disease risks based on your DNA, including your propensity for rheumatoid arthritis. More importantly, the DNA test reports provide nutrition plans and exercise suggestions that fit your unique genetic profile. When you’re armed with the right information, you can avoid inflammatory triggers and live a happier life.
References:
- Foods You Should Avoid With Rheumatoid Arthritis (Brianna McCabe) https://www.hackensackmeridianhealth.org/en/HealthU/2018/09/26/foods-you-should-avoid-with-rheumatoid-arthritis#.Y-8E_3ZBzIU
- Rheumatoid arthritis (Mayo Clinic) https://www.mayoclinic.org/diseases-conditions/rheumatoid-arthritis/symptoms-causes/syc-20353648
- Rheumatoid arthritis (RA) (CDC) https://www.cdc.gov/arthritis/basics/rheumatoid-arthritis.html
- Smoking and Rheumatoid Arthritis (Kathleen Chang et.al.) https://pubmed.ncbi.nlm.nih.gov/25479074/Everyday life with rheumatoid arthritis (Informed Health) https://www.ncbi.nlm.nih.gov/books/NBK384458/





